Meet Mr. K, an 87-year-old Chinese man recovering in a nursing home after falling and breaking his hip. Mr. K suffered from dementia and his English was weak. His wife of 50 years had passed away and his four children were unable to continue caring for him after he broke his hip. He was left in the care of a team of female caregivers who did not speak Chinese. He was in pain, confused and frightened. Many mistakes were made in Mr. K's case, resulting in the unnecessary amputation of his leg.
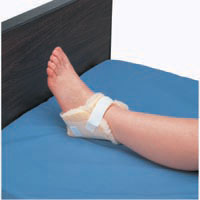
The fractured hip was not surgically repaired, as Mr. K’s heart disease made the surgery too much of a risk and the family decided not to take the chance. When he lay on his right side, Mr. K was in pain from the unrepaired fracture. In addition, he had a bunion on his left foot that was in contact with the mattress when he was side-lying. His heels were in heel protectors similar to the one pictured here:
So picture this: You have a confused 87-year-old who is in pain and is dependent on the staff members to turn him and relieve pressure by repositioning him in bed. He is lying in a bed (up until now, he had always slept on a floor) and there is a curtain around the bed that shields him from all people. Every once in a while, staff members, all female, swing open the curtain to care for him. This “caring” entails changing a diaper, washing the skin, and turning him. But Mr. K is confused and frightened. He fights off the staff members in their attempts to provide for him. He does not understand their directions. When they reposition him on his right side, he turns back to his left side as it is less painful.
Mr. K. ends up with a pressure sore, more commonly known as a bedsore, on his left foot bunion area from lying on the left side in a fetal position for long periods of time. Even after the sore develops, the pressure was not relieved from the foot. In time, the sore became infected; he had to have an amputation of his leg. The staff blamed the sore on Mr. K’s refusal to stay off his left side.
Mr. K. was in pain from his hip fracture. The nursing staff gave him an occasional Tylenol. His heel was in a heel bootie, and because he spent so much time on his side in a fetal position, the bunion area of the foot dug into the mattress causing the blood supply to cut off resulting in the death of the skin and tissue right down to the level of the bone. An infection developed in the wound that resulted in the need to amputate the leg.
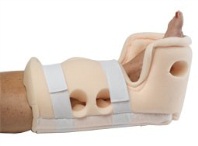
A DIFFERENT OUTCOME: All that was needed was a pillow to be placed under Mr. K.’s calf to float the foot off the surface of the bed. If the pillow was not effective, which is sometimes the case if the resident is restless, a heel elevating device similar to the one pictured here could have been utilized. You will notice that the foot “floats” inside the device and there are holes at the places where the bones protrude such as the heel, bunion area and ankle. This completely alleviates the pressure from these areas.
What are pressure sores?
According to the Mayo Clinic, “Bedsores — also called pressure sores or pressure ulcers — are injuries to skin and underlying tissues that result from prolonged pressure on the skin. Bedsores most often develop on skin that covers bony areas of the body, such as the heel, ankles, hips or buttocks. People most at risk of bedsores are those with a medical condition that limits their ability to change positions, requires them to use a wheelchair or confines them to a bed for prolonged periods.”
The skin is the major protective organ of the body. If our skin remains intact, it protects the body from infection and water loss. For the elderly, this is extremely important. When the skin is broken, germs have a new entrance to the body. This is when pressure ulcers can become fatal.
If you have a loved one living in a nursing home, chances are he or she is sedentary, either confined to a chair or a bed most of the time. What I have noticed over the years is that pressure ulcers develop right under the noses of the visitors and family members. You might be visiting your mother or grandmother in a nursing home and spending four hours with her on a Sunday. You watch her be taken from Bingo to an ice cream social and then into the day room in a wheelchair. Your loved one appears to be well dressed and bathed, and the staff members are seemingly pleasant and caring. Your loved one didn’t really want the ice cream that she had always loved; other than that you saw nothing wrong.
WHAT YOU MAY HAVE MISSED
For every one hour a person remains sedentary in a wheelchair, she should be repositioned. In the four hours you were visiting, your loved one should have been repositioned FOUR times. She also should have been taken to the bathroom as she is incontinent and was sitting in a wet diaper. While you were both enjoying the visit, injury to the skin over the buttocks or sacral area may have been occurring due to unrelieved pressure.
You left your visit feeling all was going well. But in truth, there is a good chance that a call will come informing you that there has been a complication, an ulcer has formed on the buttocks...
How to Prevent Pressure Ulcers
Here are some basic things to check on when you visit:
Are the staff members checking the skin every shift? It is quite likely that the staff asks you to leave the room when you are visiting so they can take care of the resident. If it is ok with the resident, tell the staff you are staying to look at the condition of the skin. Look for any areas of redness, abrasion-like areas, scabs, open wounds especially in areas over bones that receive pressure such as the heels, ankles, the buttocks, hips, and elbows.
Are the staff members turning and repositioning the resident every two hours while in bed?
Are the staff members repositioning the resident every hour while in the chair?
Are the heels kept off the surface of the bed? This can be done by the use of pillows or a heel lift device.
Is there a pressure relieving/reducing mattress on the bed?
Is there a pressure relieving/reducing cushion in the chair?
Ask the staff about the resident’s appetite. Is he eating and drinking sufficiently? Does your loved one look like she is losing weight?
Is the head of the bed elevated? If so, make sure the foot of the bed is cranked up so the sacral area is supported. You will know it is supported if the resident is not sliding down in the bed.
Are staff members providing frequent incontinence care (every 2-4 hours or as needed in between) to keep the skin dry and clean?
Are staff members providing moisturizer to skin after cleansing?
Are staff members providing moisture barrier if incontinent? For example, is Vaseline or Desitin being applied to the skin?
If these measures are being taken, chances are the skin will remain intact. If an ulcer does develop, hopefully it is caught at an early stage and can be healed. Once an ulcer develops, more aggressive actions need to be taken than listed above. Some things that should be done:
· Pressure should be completely avoided in an area of ulceration.
· Pressure relieving mattresses and cushions should be upgraded.
· Protein supplements may need to be given.
· More frequent skin care and observation should be conducted.
· The ulcer should be treated as directed by a physician.
· The ulcer needs to be measured and evaluated weekly to determine if there is progress or not. If there is no progress, then the care plan is either not being carried out or is ineffective and requires revisions.
· Find the nurse in charge and discuss the plan of care. Every resident/patient needs an advocate!
Some facts posted on the website of the Agency for Healthcare Research and Quality pertaining to pressure ulcers is: Number affected: 2.5 million patients per year. Cost: Pressure ulcers cost $9.1–$11.6 billion per year in the US. Cost of individual patient care ranges from $20,900 to 151,700 per pressure ulcer. Medicare estimated in 2007 that each pressure ulcer added $43,180 in costs to a hospital stay. Lawsuits: More than 17,000 lawsuits are related to pressure ulcers annually. It is the second most common claim after wrongful death and greater than falls or emotional distress. Pain: Pressure ulcers may be associated with severe pain. Death: About 60,000 patients die as a direct result of a pressure ulcer each year.
I would love to hear your comments. Please do not use names of facilities or staff members in your comments or questions. This forum is to be used to highlight the solution and provide needed information for patient/resident advocates. To receive future posts automatically, use the RSS feed in the right hand column or subscribe by entering your email address.

 RSS Feed
RSS Feed
